

07-04-2021
Post - Pandemic Hospital Design: 5 Tenets of Responsive Healthcare Ravideep Singh, Sharanya Reddy

The COVID-19 pandemic has questioned global healthcare systems. With healthcare providersstruggling to cope with unprecedented pressures, this viral outbreak has posed several newchallenges to healthcare buildings and their designers. Although many existing healthcarefacilities across the world have adapted to the changes with limited resources, somefundamental alterations in design strategies will allow us to be better prepared for futurechallenges. This article attempts to put together a set of guidelines for a possible trajectory the‘Post Pandemic’ hospital design should follow. The five tenets of responsive healthcare are:

1.Strategic Site Location:
Sites for the development of healthcare facilities are typically selected based on financialfeasibility, patient catchment, service area assessments, etc. However, an essential factor that developers should also consider is the availability of vacant areas or adjacent infrastructure that can be utilised as transitional ‘flex’ facilities. These ‘flex’ spaces will allow hospitals to usesurrounding areas to accommodate the increase in patient -care requirements during unprecedented outbreaks or pandemics by multiplying beds or setting up Alternate Care Facilities. These spaces will also facilitate seamless access to critical hospital functionalities such as the ORs, high-intensity radiation equipment, etc., thereby resulting in enhanced care delivery and serving a much larger community.
2.Planning for Flexibility and Reconfiguration:
The present planning trends tend to gravitate towards a cost-effective model to reduce the upfront investments rather than factoring for influx capacities during an outbreak or pandemic.There is a pressing need for developing scenarios during the financial planning stage that incorporates the capabilities of a healthcare facility to respond to unanticipated circumstances.
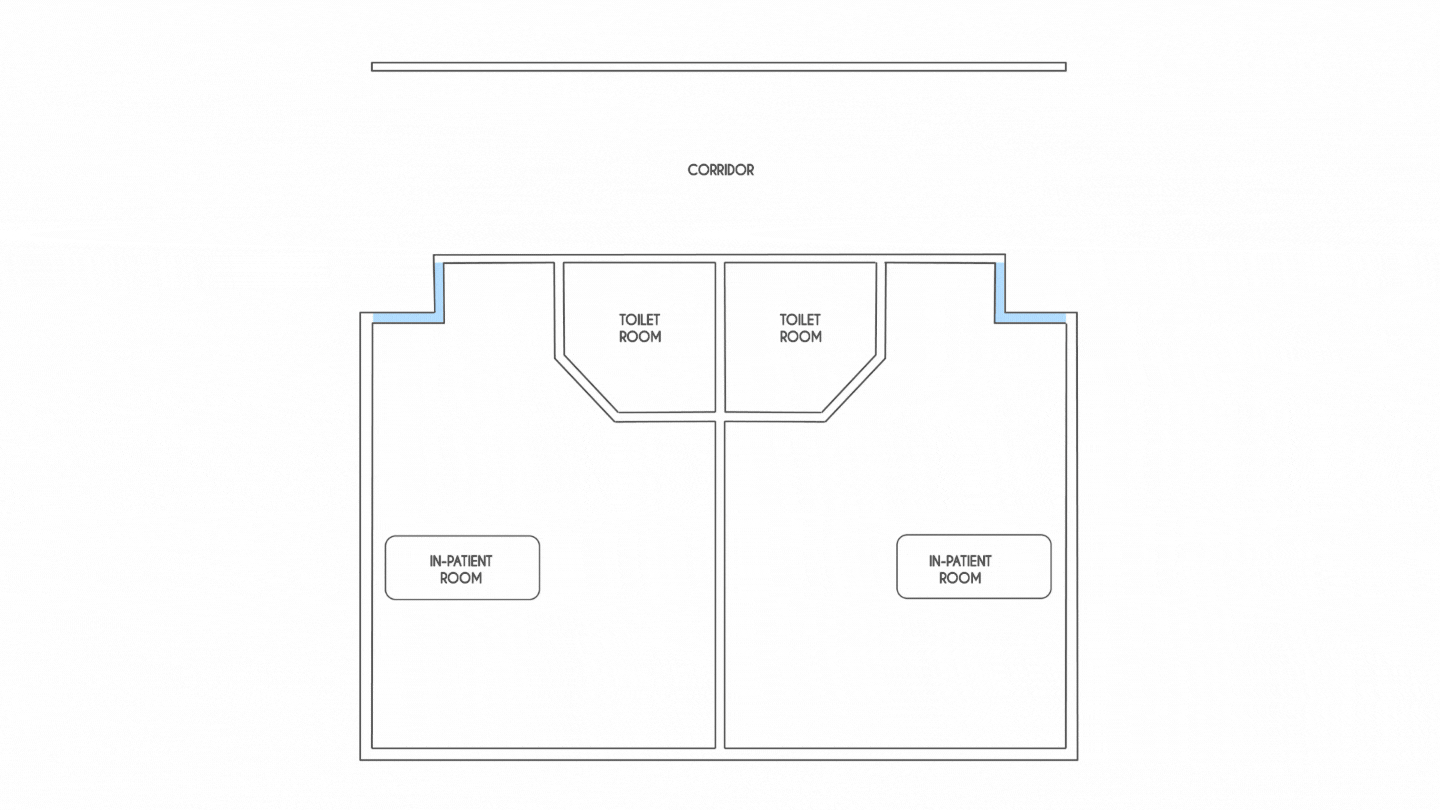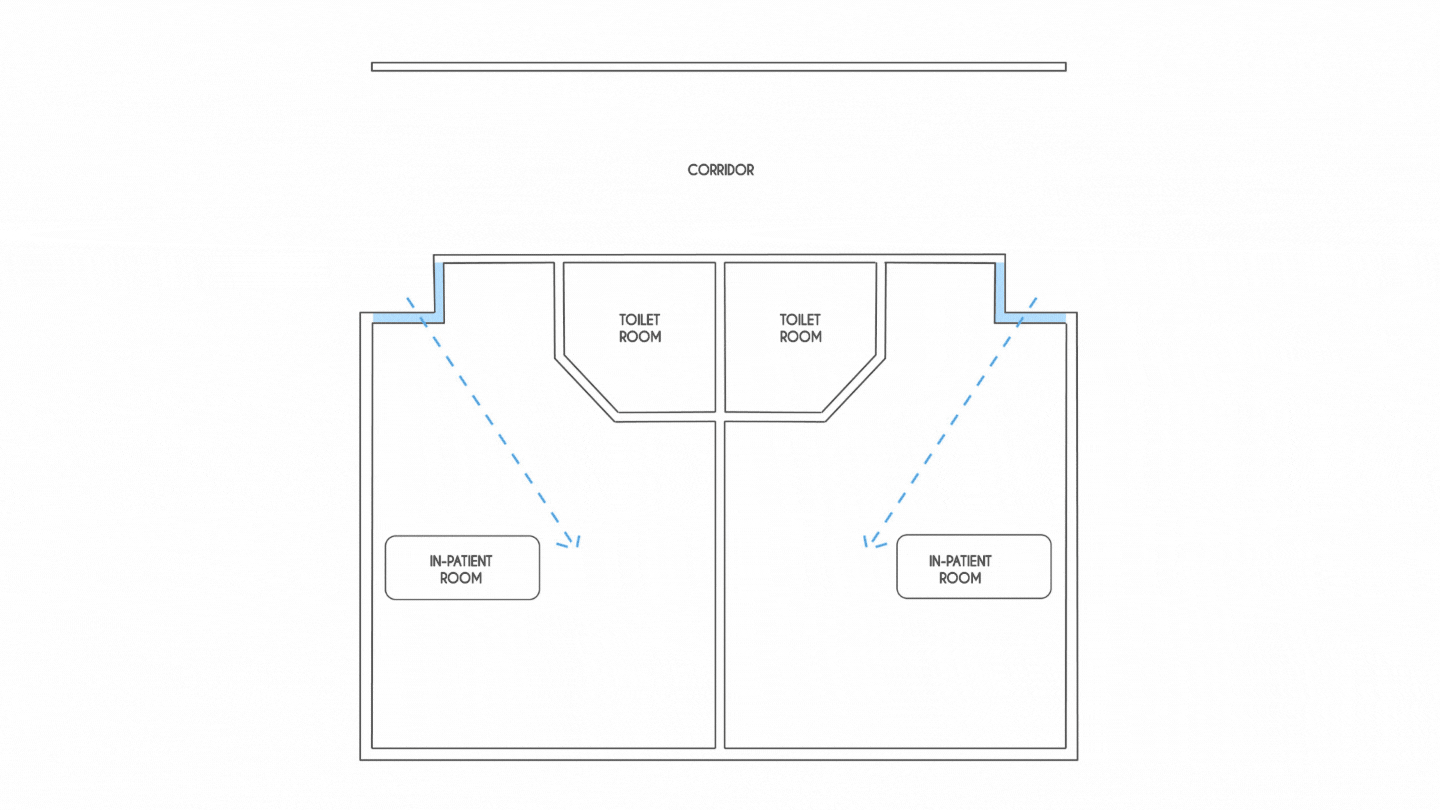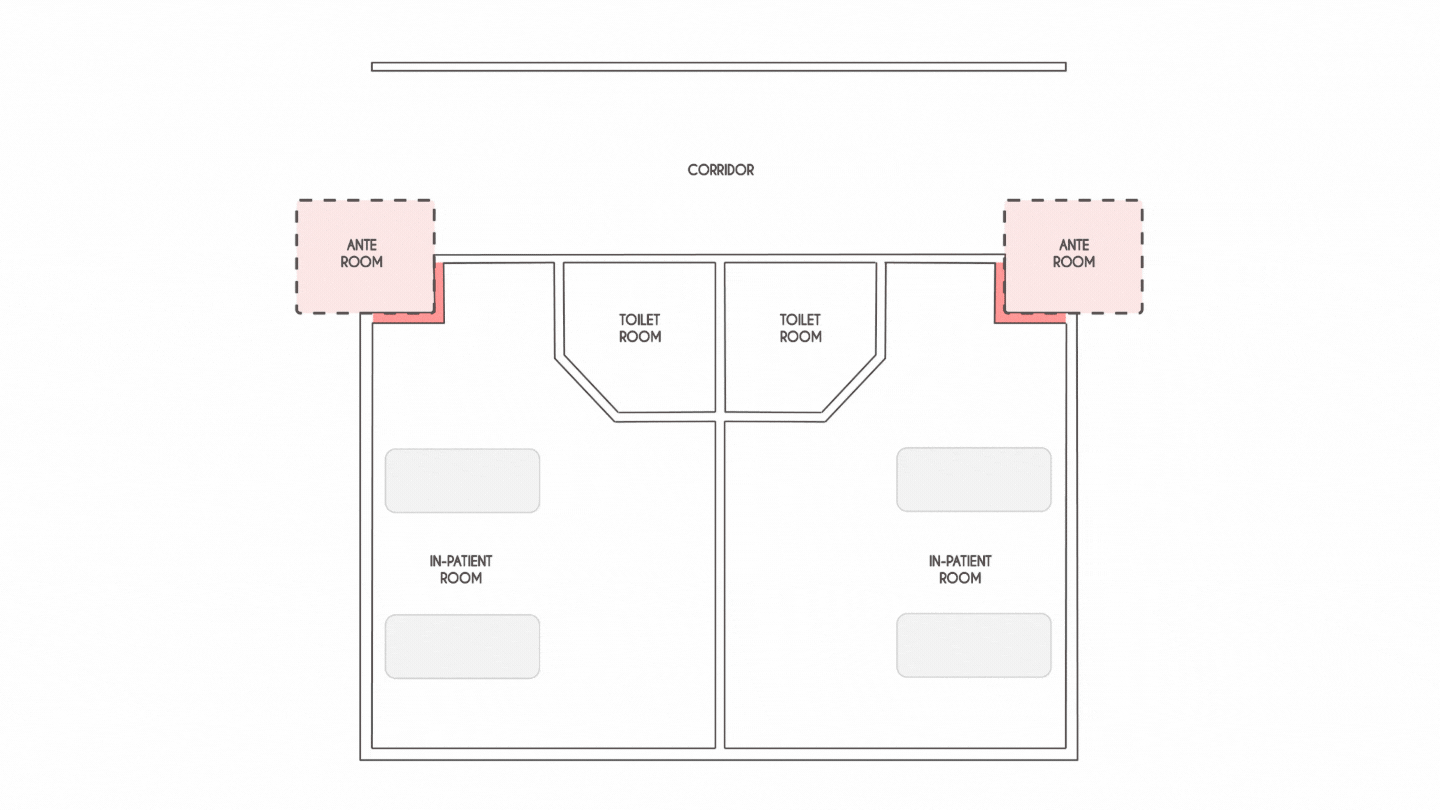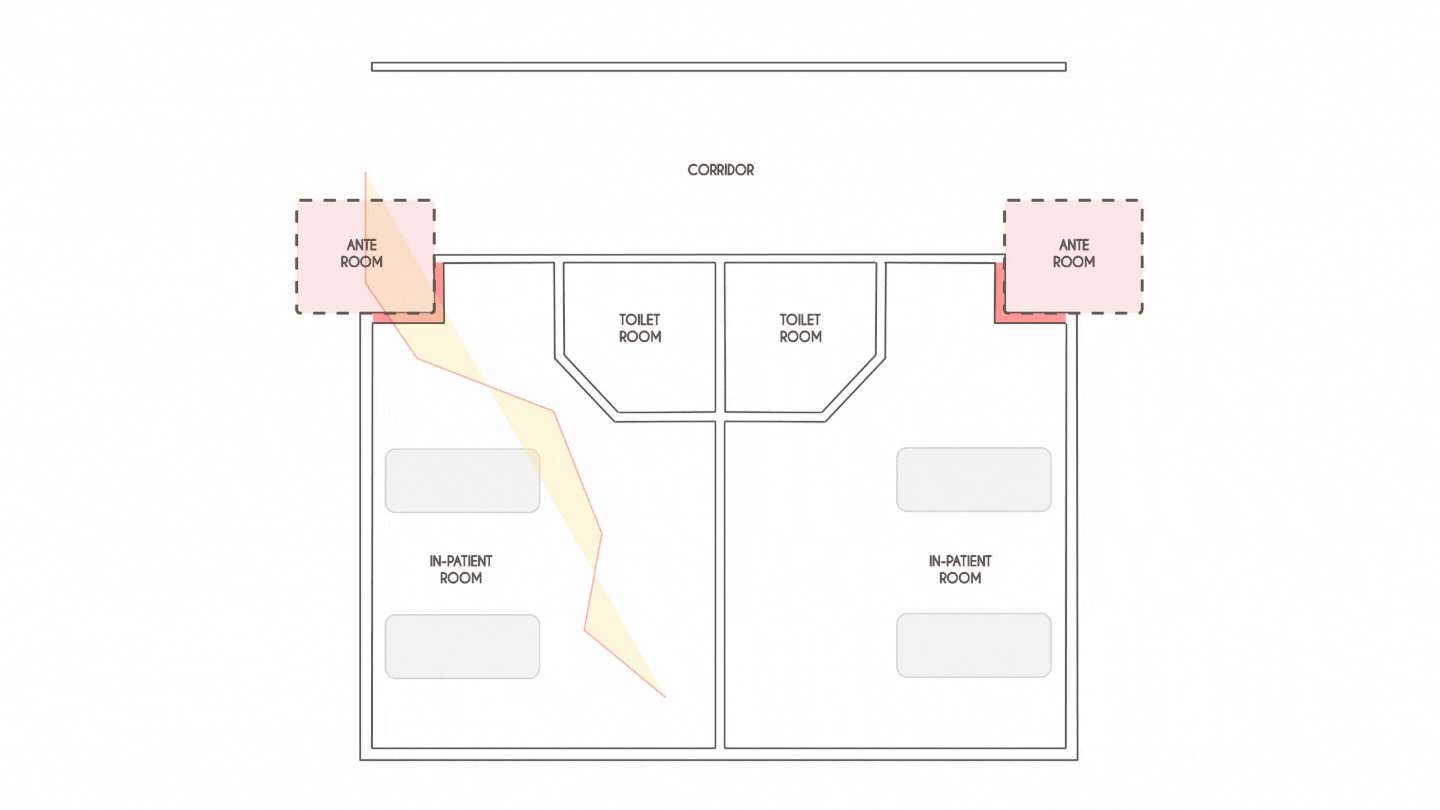
Spatial flexibility and planning will be the most critical factor that will drive healthcare design in the coming years. For instance, IPD rooms planned on a 33 ft grid that can accommodate two patients in a room allow for flexibility to add portable HEPA filters to anterooms in corridors,thereby moulding each patient room into a negatively pressurised unit.
At the onset, the pandemic witnessed a drastic increasein the need for ICUs. Hence, creating adaptive spaces that can be reconfigured into ORs, PACU, perioperative bed or other administrative areas is a possible design strategy that could accommodate critically ill patients.Developing medical planning scenarios during the design stage that determine the maximum surge capacity should also be thoughtfully considered.

3.Planning for segregation:
During a pandemic outbreak, healthcare facilities should ensure the segregation of infectious,non-infectious and creating a forward triage area within the building. Considering the need to isolate patients, healthcare planners and stakeholders should simulate experimental zoning scenarios and develop strategies for an effective response. These scenarios could attempt to isolate areas meant for infectious and non-infectious patients while also allowing the healthcare staff to operate and cater to all zones seamlessly.
Pre-planning these zones in such a manner allows for easy implementation and execution of workflows in any scenario, thereby equipping the hospital to adapt and respond promptly and effectively. It is also important to note that incorporating these strategies while planning may not affect the initial investment but will result in a better response rate during a pandemic or an outbreak.
4.Variable Mechanical Support System:
In addition to the planning and segregation of various zones, it is vital to select the correct type of mechanical equipment used in the infectious and non -infectious areas within the hospital.HVAC systems that have variation capacity should be considered to improve air-exchange rates allowing required zones to function as negatively pressurised spaces whenever needed.Designing smoke compartments to double up as isolated negatively pressurise d units is another planning strategy that allows for segregation without any significant upfront investment.
5.Implementation of Tele-health:
The COVID-19 pandemic has compelled a large number of people to identify and utilise the technology to work remotely .This has allowed for the telehealth market to expand and grow globally. The United States Telehealth market alone witnessed a whopping 80% growth in 2020,making it a USD 9.5 billion industry. With these statistics, it has become imperative for health facilitators to account for optimum technological and infrastructural apparatus for telehealth facilities in the hospitals to grow exponentially, rendering higher magnitudes of care delivery.
These proposals have elicited from the lessons learned by various healthcare providers who have struggled to make their way through the adversities of the COVID -19 pandemic and attempts to initiate a comprehensive and responsive healthcare design dialogue.













